This is part of a continuing series on provider data, compliance, and the revenue cycle
Previous articles in this series: When Your Provider Directory Becomes Public Infrastructure | The REAL Health Providers Act Is Not Hypothetical | Provider Directories Aren’t Just a Compliance Problem—They’re a Revenue Cycle Problem | Provider Data Errors Don’t Stop at the Directory—They Break the Revenue Cycle
Provider data is not static.
Addresses change. Phone numbers are reassigned. Providers relocate, retire, merge practices, or shift network participation. Acceptance status fluctuates. Taxonomy designations are updated. Credentialing lapses.
Yet many organizations still govern provider data as though it were a fixed asset rather than a living system. That mismatch is the root cause of data drift: the gradual, compounding divergence between what your systems say and what operational reality actually reflects.
Drift Is Structural, Not Operational
The evidence here is not anecdotal. Peer-reviewed research published in the American Journal of Managed Care followed provider directory listings over an extended period and found that inaccuracies persisted across all carriers and specialties studied, with approximately 40% of providers originally identified as inaccurately listed still showing at least one inaccuracy after an average of 540 days, despite regulatory pressure and awareness.
This is not a failure of diligence. It is a structural reality.
When dynamic data is governed by periodic processes, divergence is inevitable. The Minnesota Department of Health’s Provider Directory Feasibility Study, commissioned by the state legislature to assess the viability of a centralized statewide directory, confirmed that maintaining accurate directories is “very time and resource intensive” and that data accuracy “will always be a challenge” without continuous verification and provider engagement mechanisms.
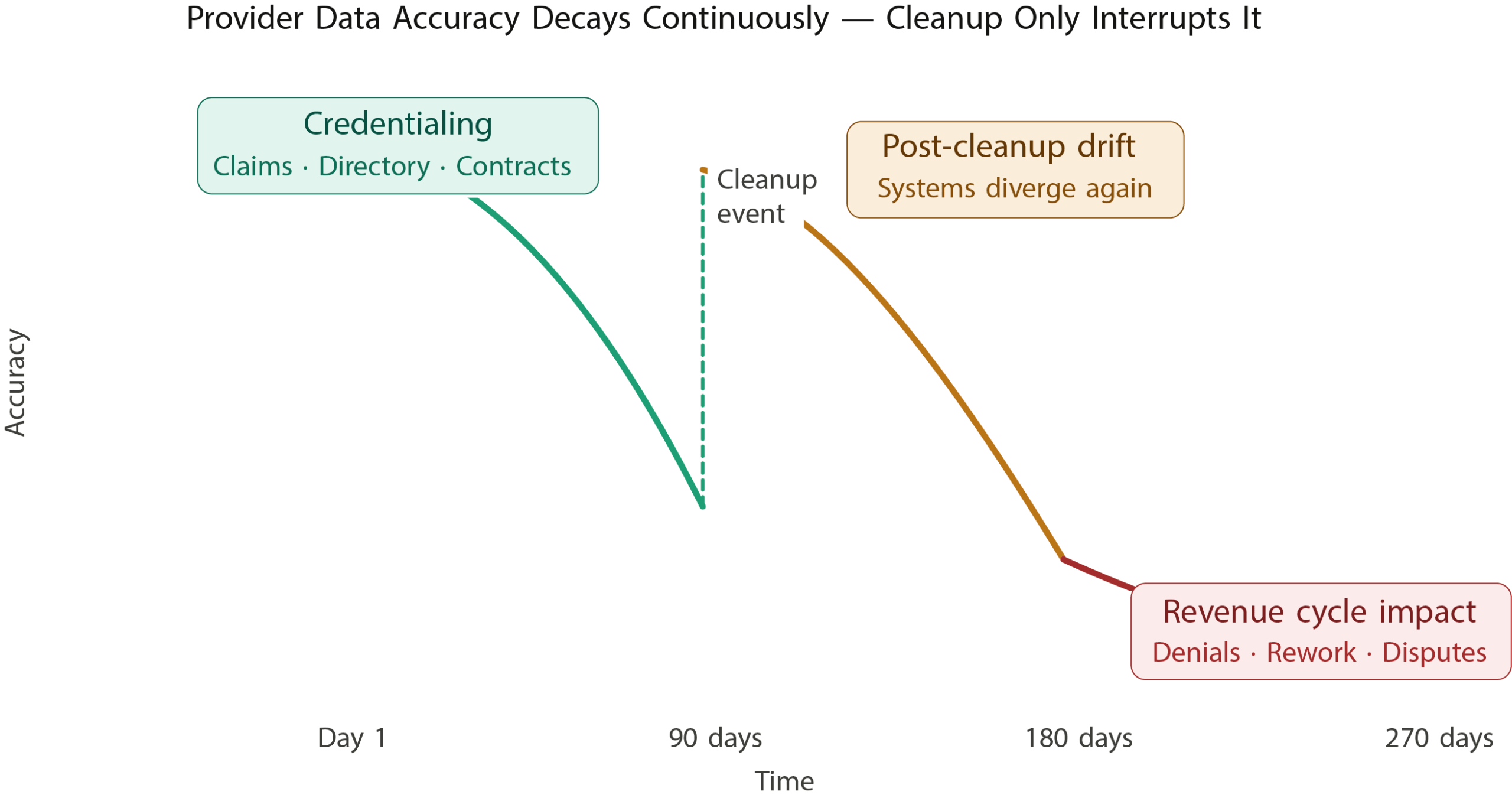
What is particularly instructive from both bodies of research is this: cleanup efforts do not arrest drift. They interrupt it. The degradation resumes the moment the process does.
The Cleanup Illusion
Most organizations operate on a familiar cycle:
- Inaccuracy is identified — often through a denial, a complaint, or a regulatory audit
- An intensive reconciliation effort is launched
- Temporary restoration of alignment is achieved
- Gradual degradation resumes
- The cycle repeats — typically under heightened scrutiny and compressed timelines
Cleanup improves the snapshot. It does nothing to stabilize the system.
Research from CAQH captures the scope of the underlying burden. A typical physician practice must respond to directory update requests from approximately 20 health plans, each through separate platforms, formats, and timelines. That fragmented process creates a nearly constant stream of administrative work that undermines the very data quality it is meant to improve.
And because providers are often contacted by multiple plans simultaneously, different staff members respond with inconsistent answers. Sometimes to the same question from the same plan at different points in time. The process designed to fix the problem is, in part, generating new errors.
Why This Now Reaches the Revenue Cycle
In previous articles in this series, we established that provider data errors do not stop at the directory, they propagate directly into claims systems, adjudication logic, and payment workflows. That connection becomes even more consequential when you layer in drift.
Stale or degraded provider data flowing into revenue cycle systems creates a compounding problem:
Claims routing errors. When a provider’s network participation status is outdated, claims are routed against incorrect adjudication logic, triggering denials that reflect the state of the data at a prior point in time, not the current contractual reality.
Reimbursement misalignment. Incorrect taxonomy designations or specialty classifications result in wrong reimbursement rates being applied. The payer pays incorrectly. The provider disputes. The cycle consumes staff time at both ends.
Auto-adjudication suppression. The 2024 CAQH Index identifies a $20 billion savings opportunity available to the industry through automation of administrative workflows. That opportunity is structurally inaccessible when provider records are inconsistent or stale, because claims fall out of straight-through processing and into manual review queues.
Rework and appeals cost. As established in prior research, reworking a denied claim costs anywhere from $25 to $181 per claim. Provider-data-driven denials ( those stemming from incorrect identifiers, outdated locations, or taxonomy mismatches), are among the most avoidable category of denials in the revenue cycle. They are also among the most persistent, because their root cause is upstream infrastructure, not downstream workflow.
Risk adjustment exposure. The connection between provider data quality and revenue integrity runs deeper than most organizations track. Healthscape Advisors has documented cases where inaccurate provider records directly suppressed risk adjustment performance, in one instance, a regional health plan discovered that more than 40% of claims were being mistakenly denied due to inaccurate provider data, a failure mode that breaks the attribution logic underlying accurate risk adjustment and HCC coding. When providers are misidentified, misclassified, or unresolvable across systems, diagnosis capture fails and the revenue consequence is permanent, not recoverable through appeals.
Each of these is a revenue cycle outcome. Each has a provider data infrastructure problem at its root. And all of them worsen proportionally as drift velocity increases and the interval between cleanup cycles lengthens.
Why This Matters More Now
Regulators no longer treat directory accuracy as an internal compliance artifact. They treat it as a consumer protection obligation — and increasingly as a financial integrity question.
That means drift is no longer a background operational issue absorbed quietly by revenue cycle teams. It is a visible risk vector with measurable consequences:
- Regulatory findings and corrective action plans
- Member complaints and member abrasion
- Litigation exposure (as this series has documented, $45M+ in settlements in 2025 alone)
- Suppressed auto-adjudication rates
- Executive and board-level accountability
And the more complex the operating environment, credentialing systems, contracting databases, claims platforms, delegated rosters, third-party vendors, the faster drift compounds. Periodic remediation cannot keep pace with systemic divergence across a multi-layered infrastructure.
A particularly instructive data point: research from Virsys12 and IDC found that healthcare organizations lose an average of $2.4 million annually due to provider data inaccuracies alone; costs that accumulate across manual verification, compliance penalties, reprocessing, and missed market opportunity.
That figure does not include the upstream suppression of auto-adjudication performance, the downstream cost of denied claim rework, or the revenue leakage from risk adjustment exposure. It is the visible portion of a larger number.
Continuous Validation Is Not a Feature
It is an architectural requirement.
Continuous validation means:
- Ongoing reconciliation across credentialing, contracting, claims, and directory systems — not sequential handoffs
- Real-time identity resolution that resolves the same provider appearing differently across platforms
- Drift detection before it reaches claims systems and generates denials
- Structured exception governance with closed-loop correction upstream, not just at display layers
- Evidence trails that support regulatory defensibility without additional manual effort
It treats provider data as a living infrastructure layer — not a file to be refreshed on a quarterly schedule.
Organizations that redesign around this principle shift from reactive correction to systemic stability. Their revenue cycle teams stop absorbing the downstream cost of upstream data problems. Their compliance posture reflects continuous accuracy rather than periodic attestation. Their auto-adjudication rates reflect the quality of their data infrastructure, not the competence of their claims staff.
Organizations that do not make this shift will continue to fund repetitive cleanup cycles under increasing regulatory scrutiny, rising litigation exposure, and compounding rework costs that are difficult to isolate and nearly impossible to eliminate without addressing the root architecture.
The Executive Question
The C-suite decision is not whether cleanup works. It does. Temporarily.
The question is whether your organization is architected to prevent re-divergence.
If your accuracy model depends on episodic intervention, drift is already occurring. And the longer it goes unmeasured, the more expensive it becomes — across compliance, claims operations, and revenue cycle performance simultaneously.
Executive teams should be asking:
- Where does drift originate in our architecture — and how many systems does it touch before it generates a denial?
- How quickly does accuracy decay post-cleanup, and are we measuring that velocity?
- How many FTEs are currently absorbing the cost of upstream data fragmentation inside our revenue cycle?
- Are we validating continuously — or auditing periodically and hoping the interval is short enough?
Provider data is no longer a back-office function. It is regulated infrastructure with direct revenue implications.
The costs of drift are not always visible in a single metric. They accumulate across compliance exposure, auto-adjudication suppression, claims rework, payment disputes, and risk adjustment integrity. Most organizations can quantify their compliance costs. Few can quantify their divergence velocity or the full revenue cycle impact of the gap between their last cleanup and today.
If you want to understand how drift is silently compounding operational expense, regulatory exposure, and downstream rework in your organization, let’s talk. No demo. No sales pitch. Just a 30-minute strategy session to share perspective and help you quantify what misalignment is actually costing your organization.
We invite you to learn more through the key sources referenced in this article:
- AJMC — Persistence of Provider Directory Inaccuracies After the No Surprises Act
- Minnesota Department of Health — Provider Directory Feasibility Study
- CAQH — Hidden Causes of Inaccurate Provider Directories (Whitepaper)
- CAQH — 2024 Index Report
- Change Healthcare — 2022 Revenue Cycle Denials Index
- HealthScape Advisors – 4 steps to address data accuracy challenges for health plans
- Virsys12 / IDC — The Hidden Costs of Inaccurate Provider Data