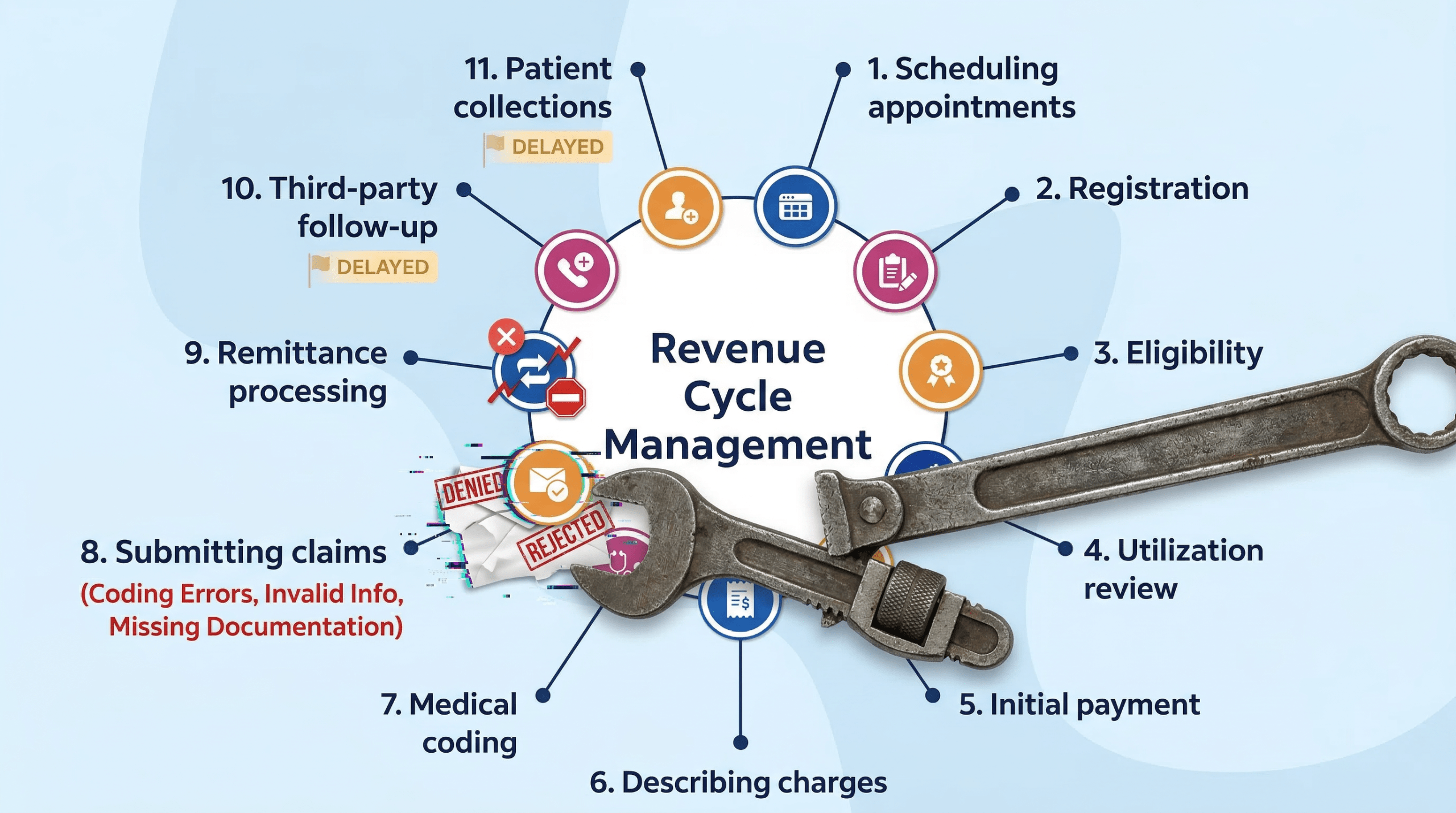
Why inaccurate provider data quietly disrupts claims, payments, and operations
Provider directory accuracy is often framed as a compliance obligation.
Operational leaders know it is more than that.
The same fragmented provider data that creates inaccurate directories also propagates through the healthcare revenue cycle, affecting claims routing, eligibility checks, reimbursement accuracy, and payment timing.
In other words, the problem does not end with the directory.
It permeates the entire revenue cycle and can wreak havoc on financial operations.
Provider Data Sits at the Center of Multiple Financial Workflows
Provider data flows through far more systems than most organizations realize.
It is referenced by:
- Network contracting systems
- Credentialing databases
- Claims processing platforms
- Eligibility verification engines
- Payment integrity tools
- Provider directories
- Recruiting systems
Each system often maintains its own version of provider identity and attributes.
Industry analysis consistently shows that provider information is fragmented across multiple administrative systems, creating discrepancies that affect both compliance and operational processes. (Source: CAQH — Index Report on Administrative Simplification)
When these systems disagree about provider identity, location, specialty, or network participation, the revenue cycle becomes vulnerable to disruption.
Claims are not denied because directories are inaccurate.
Claims are denied because the same inaccurate data appears inside claims systems.
Small Provider Data Errors Create Large Financial Consequences
Even minor discrepancies in provider records can cascade through the revenue cycle.
Examples include:
- Provider identifiers mismatched across systems
- Outdated practice locations
- Incorrect specialty designations
- Inconsistent network participation status
When these attributes do not reconcile across systems, common outcomes include:
- Claims routed to the wrong network logic
- Incorrect reimbursement rates applied
- Claims flagged for manual review
- Payment delays while provider records are reconciled
Revenue cycle research consistently shows that inaccurate or incomplete provider information contributes to claim rework, manual intervention, and administrative cost. (Source: Change Healthcare — 2022 Revenue Cycle Denials Index)
While the root cause is data fragmentation, the operational symptom appears as denials, appeals, and delayed payments.
Administrative Rework Is the Hidden Cost
The financial impact of inaccurate provider data rarely appears as a single metric.
Instead, it accumulates through operational friction:
- Claims flagged for manual review
- Payment corrections and adjustments
- Reprocessing cycles
- Call center escalations
- Provider disputes
The CAQH Index estimates that the U.S. healthcare system spends tens of billions of dollars annually on administrative inefficiencies tied to manual workflows and data fragmentation.
Provider data inconsistencies are one of the structural drivers behind that administrative burden. Each unresolved discrepancy introduces another manual touch in the revenue cycle.
Revenue Cycle Teams End Up Solving Data Problems
When provider records do not reconcile upstream, the downstream systems compensate.
Revenue cycle teams often find themselves resolving issues that originate in provider data infrastructure:
- Investigating claims mismatches
- Verifying network participation manually
- Reconciling provider identifiers across systems
- Correcting payments after adjudication
From a financial perspective, these are not revenue cycle problems.
They are data architecture problems appearing inside the revenue cycle.
Compliance Risk and Financial Risk Are Now Converging
Historically, inaccurate provider data was treated as a compliance exposure tied to directories and regulatory oversight.
Today, the operational reality is broader.
The same data inconsistencies now influence:
- Regulatory compliance
- Member access accuracy
- Claims processing integrity
- Provider reimbursement workflows
What appears externally as a directory issue internally becomes a revenue cycle efficiency problem. Organizations that treat provider data solely as a compliance obligation often underestimate its financial impact.
Questions Revenue Cycle Leaders Should Be Asking
For CFOs, COOs, CIOs, and Revenue Cycle leaders, the key questions are not about directory accuracy alone.
They are about operational integrity across the financial workflow.
Consider asking:
- How often do provider data discrepancies trigger claim rework?
- How many claims require manual intervention due to provider mismatches?
- How often are payments adjusted due to incorrect provider attributes?
- How many operational teams are compensating for data inconsistencies upstream?
If revenue cycle teams are frequently resolving provider data discrepancies, the problem is not downstream.
The problem is structural.
The Strategic Implication
Provider data is often treated as a compliance artifact. In reality, it functions as a core financial data layer inside the healthcare enterprise.
When that layer is fragmented, operational teams compensate by performing manual intervention, reconciliation, and payment corrections.
When it is governed and reconciled continuously, the revenue cycle operates with far less friction.
For healthcare leaders, the implication is clear: Improving provider data accuracy is not just about avoiding regulatory scrutiny. It is about protecting the operational integrity of the revenue cycle.
When you’re ready to proactively make the necessary changes to protect your revenue cycle, let’s talk.
No demo. No sales. Just a 30-minute discussion to share ideas and maybe hear a different perspective on the issue.